Screening
Diagnosis

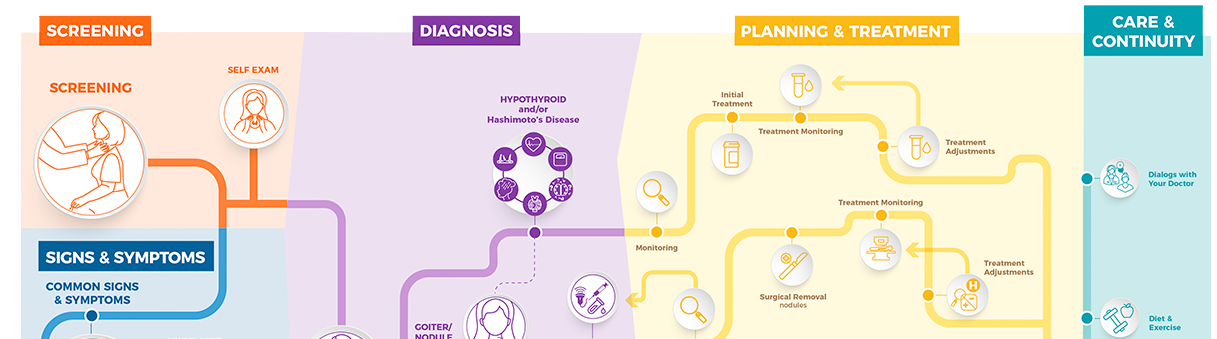
Thyroid Disease Diagnosis
How are thyroid disorders diagnosed?
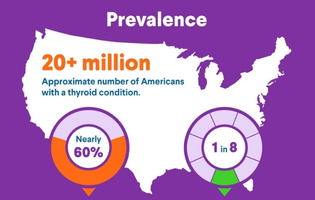
Thyroid disease affects as many as 20 million Americans, and more than half remain undiagnosed because symptoms are often similar to the signs of other medical conditions. If you're experiencing any symptoms, the first step is to speak with a health care professional to see if a thyroid test is needed to check your thyroid gland.
There are several types of tests to help determine if you have a thyroid problem. Below is an overview of the tests used to diagnose common thyroid conditions.
 Hypothyroidism
Hypothyroidism
Hypothyroidism
An underactive thyroid, or hypothyroidism, occurs when the thyroid gland creates less than the normal amount of thyroid hormone. The result is the “slowing down” of many bodily functions. Hypothyroidism usually is a permanent condition that can be treated. Of the nearly 20 million people estimated to be suffering from thyroid dysfunction, most have hypothyroidism.
Symptoms and physical signs can signal hypothyroidism. However, the condition may develop slowly, so many people do not realize that their body has changed. A primary care provider may make the diagnosis of hypothyroidism, but assistance is often needed from an endocrinologist, a specially trained health care professional who is qualified to diagnose and treat hormone-related conditions, including diseases related to the thyroid gland.
Hypothyroidism testing may include:

- TSH (thyroid-stimulating hormone or thyrotropin): An increased TSH level in the blood is the most accurate indicator of hypothyroidism. Production of TSH is increased when the thyroid gland even slightly underproduces thyroid hormone.
- Estimates of free thyroxine (T4) test: This measures the level of T4 in your blood.
- Thyroid antibodies: Indicates the likelihood of autoimmune thyroiditis being the cause of hypothyroidism.
Hashimoto's Disease
Hashimoto's thyroiditis (also called Hashimoto's disease or chronic lymphocytic thyroiditis) is the most common thyroid disease in the United States. It is about seven times more common in women.
Hashimoto's disease involves the production of immune cells and autoantibodies by the body's immune system that can damage thyroid cells and compromise their ability to make thyroid hormone. Hypothyroidism occurs if the amount of thyroid hormone produced is not enough for the body's needs. The thyroid gland may also enlarge, forming a goiter.
Hashimoto's disease testing may include:

- Anti-thyroid antibodies: Testing for increased anti-thyroid antibodies (usually anti-thyroid peroxidase or anti-thyroglobulin antibodies) can confirm Hashimoto's disease, but the antibodies are not present in all cases.
- TSH (thyroid-stimulating hormone or thyrotropin): Increased TSH level in the blood is the most accurate indicator of hypothyroidism. The level of TSH rises dramatically when the thyroid gland underproduces thyroid hormone.
- Estimates of free thyroxine (T4) test: This measures the level of T4 in your blood. A low level of free T4 is consistent with thyroid hormone deficiency. However, free T4 values "within typical limits" may still represent thyroid hormone deficiency in a particular person, since a high level of TSH stimulation may keep the free T4 levels "within typical limits" for many years.
 Goiter, Nodules, and Thyroid Cancer
Goiter, Nodules, and Thyroid Cancer
Goiter
If your thyroid increases in size, your health care professional may diagnose you with a goiter. A goiter is, quite simply, an enlarged thyroid. Your health care professional may discover a goiter during a checkup, when they examine your thyroid by feeling (palpating) your neck. Or a goiter may show up on imaging tests. You may develop a goiter when your entire thyroid swells up and becomes enlarged, or a goiter may occur when your thyroid grows one or more lumps, known as nodules.
There are several types of goiter, including:
- Simple goiter: A goiter that occurs when your entire thyroid gets larger. This is also known as a diffuse goiter.
- Nodular goiter: A goiter that contains a single thyroid nodule.
- Multinodular goiter: A goiter that contains several nodules.
- Endemic goiter: A goiter caused by a deficiency of the mineral iodine.
Nodules
Thyroid nodules are lumps that develop in or on your thyroid. Most thyroid nodules are benign (not cancerous). In fact, only 10 to 15 percent of thyroid nodules contain cancer cells. Your health care professional may discover a thyroid nodule during a checkup when they examine your thyroid by feeling (palpating) your neck. Or a nodule may show up on imaging tests. A nodule may be so small that your health care professional can't feel it, or large enough that it is visible to you or others looking at your neck. You may develop a single nodule or several nodules.
If your health care professional feels a goiter in your neck, or discovers one or more nodules on your thyroid, they typically order testing to learn more. Having a goiter or nodule is not the same as having thyroid cancer. In fact, most goiters and nodules are benign (not cancerous).
Thyroid Cancer
Only a small percentage of thyroid nodules are cancerous. Thyroid cancer is a malignant tumor or growth originating within the thyroid gland. Most types of thyroid cancer are treatable, and patients go on to live long, healthy, normal lives. For more information about thyroid cancer, visit our partner organization, ThyCa: Thyroid Cancer Survivors’ Association.
Goiter/nodule/thyroid cancer testing may include:

- Blood tests: Thyroid blood tests check for irregular levels of thyroid hormones in your blood. Your health care professional may test your TSH thyroxine (T4), and sometimes triiodothyronine (T3). You may also receive a blood test for antibodies that affect your thyroid's function.
- Imaging: Your health care professional may recommend imaging tests such as ultrasound, which uses sound waves to create images of your thyroid. Imaging tests provide more information about the size of your goiter and whether it contains nodules.
- Radioactive iodine uptake: If your health care professional suspects certain types of thyroid disease, such as Graves' disease, they may recommend a test that uses a small amount of radioactive iodine and imaging to check for overactivity.
- Thyroid scan: This is a test that creates images of your thyroid using a small dose of a radioactive isotope. The results of this test give your health care professional important information about whether or not the nodule is making too much thyroid hormone.
- Biopsy: In the event thyroid nodules are found, sometimes a biopsy using a fine needle to remove a small sample of your thyroid to check it for the presence of cancer cells if necessary.
 Hyperthyroidism and Graves' Disease
Hyperthyroidism and Graves' Disease
Hyperthyroidism
Hyperthyroidism occurs when the body makes too much thyroid hormone. This disorder occurs in almost 1% of all Americans and affects women 5 to 10 times more often than men. In its mildest form, hyperthyroidism may not cause recognizable symptoms. More often, the symptoms are uncomfortable, disabling, or even life-threatening. A trained health care professional can identify characteristic symptoms and physical signs of the disease. Tests can be used to confirm the diagnosis and to determine the cause.
Graves' Disease
Graves' disease is an autoimmune disorder that causes the immune system to overstimulate the thyroid gland and produce too much thyroid hormone. This can eventually cause hyperthyroidism (overactive thyroid). Graves' disease is the most common cause of hyperthyroidism in the United States and is 7 times more likely to affect women.
Hyperthyroidism and/or Graves' disease testing may include:

- TSH (thyroid-stimulating hormone or thyrotropin): A low TSH level in the blood is the most accurate indicator of hyperthyroidism. The body shuts off production of this pituitary hormone when the thyroid gland even slightly overproduces thyroid hormone. If the TSH level is low, it is very important to also check thyroid hormone levels to confirm the diagnosis of hyperthyroidism.
- Estimates of free thyroxine (T4) and free triiodothyronine (T3): This measures the levels of active thyroid hormones in the blood. When hyperthyroidism develops, free T3 and free T4 levels rise (although they may still be within the normal range for the general population) and are often considerably higher than normal.
- TSI (thyroid-stimulating immunoglobulin) and/or TRAb (thyrotropin receptor antibodies): These antibodies are often found in the blood when Graves’ disease is the cause of hyperthyroidism.
- Radioactive iodine uptake (RAIU): a measurement of how much iodine the thyroid gland can collect, and thyroid scan, which shows how the iodine is distributed throughout the thyroid gland. This information can be useful in determining the cause of hyperthyroidism and, ultimately, its treatment.
- Imaging: Ultrasound, and occasionally CT or MRI scans can be used to look at your thyroid.
- Referral to an eye doctor: If your health care professional suspects you have Graves' ophthalmopathy (thyroid eye disease), you may be referred to an ophthalmologist.
 Thyroid Eye Disease
Thyroid Eye Disease
Thyroid Eye Disease
Thyroid eye disease is an autoimmune disorder that causes your immune system to mistakenly attack the tissues behind your eyes. Sometimes people who have Graves' disease may also develop thyroid eye disease over time. A variety of factors including, genetics, the environment, and smoking, may cause or worsen thyroid eye disease.
If you are newly diagnosed with thyroid eye disease, your eye doctor may ask you to see an endocrinologist to check your hormone levels.
Thyroid eye disease testing may include:

- Blood tests: used to check your thyroid levels and thyroid antibodies
- Imaging: CT or MRI of the eyes can be used to examine swelling tissue behind the eye
- Vision testing
- Color vision testing
- Visual field testing
- Eye measurements
- Eye pressure readings
- Optic nerve tests
Undiagnosed thyroid issues can increase the risk for other serious conditions, such as cardiovascular disease, obesity, osteoporosis, and infertility. However, most thyroid diseases are lifelong conditions that can be managed with medical attention. The first step is to talk with a health care professional or endocrinologist to ensure your thyroid gland is healthy and functioning properly. Your health care professional will help determine which tests are the most appropriate for your situation.





 DOWNLOAD
DOWNLOAD