Obesity Glossary
A
Adiposity-based chronic disease (ABCD): Another name for obesity. Rather than focusing just on weight, ABCD takes into account the health impact of excess weight, such as type 2 diabetes, heart disease, stroke, and some types of cancers. This term identifies obesity as a chronic disease, places the focus on the health risks of having excess weight or adipose tissue (body fat), and avoids the stigma associated with the term "obesity."
B
Bariatric surgery: Any type of surgical procedure performed on the stomach and/or intestines to help bring about long-term weight loss. Also known as obesity surgery.
Behavioral substitution: A behavioral-therapy strategy where you substitute an overeating behavior with a healthier behavior, such as going for a walk when you feel stressed instead of snacking.
Behavioral therapy: The name used for a wide range of behavior-change techniques that focus on adjusting your ingrained lifestyle habits, especially those related to eating and physical activity. Examples of behavioral therapy include goal setting, stimulus control, behavioral substitution, cognitive restructuring, and joining a support group. Also known as behavioral counseling.
Biliopancreatic diversion with duodenal switch: A type of obesity surgery that combines a sleeve gastrectomy surgery and gastric bypass surgery. Also known as "mixed surgery."
Body mass index (BMI): A screening tool that uses your height and weight to determine if you are underweight (BMI less than 18.5), of healthy weight (BMI between 18.5 and 25), overweight (BMI between 25 and 30), or obese (BMI 30 or above). BMI provides a quick estimate of body fat and is not affected by age, gender, or race. However, it does not account for factors such as muscle mass, age, sex, or location of fat in your body.
C
Chronic disease: A medical condition that requires ongoing care and/or treatment. Examples of obesity-related chronic diseases include type 2 diabetes, high blood pressure, and cardiovascular disease.
Cognitive restructuring: A behavioral/psychological therapy strategy where you replace distorted thinking with more realistic perspectives. Some mental health care professionals specialize in cognitive restructuring.
D
Dumping syndrome: A condition that may occur in people who undergo obesity surgery. It can cause symptoms such as flushing, rapid heart rate, abdominal pain, vomiting, and diarrhea. Dumping syndrome can usually be prevented by eating protein-based meals and avoiding simple carbohydrates.
Dysregulated eating: Abnormal eating behaviors, including bulimia, anorexia nervosa, binge eating, and purging. Because these behaviors can make it harder for you to recognize your body's hunger and fullness signals, they may lead you to overeat and gain excess weight. Also known as eating disorders or disordered eating.
E
Endocrinologist: A physician who has received specialized training in diagnosing and treating hormone-related diseases and conditions, including obesity, thyroid disease, osteoporosis, diabetes, infertility, and adrenal disorders.
F
Five A model: A model that your health care professional may use to support you on your weight-management journey. It was first developed to help people quit smoking, but its success led health care professionals to apply it to weight loss as well. It includes five actions: ask, assess, advise, agree, and assist.
G
Glucose: The main source of energy or fuel for all of your body's functions. Although your body gets most of its glucose from carbohydrates in food, glucose can also be made from protein and fat. People with diabetes have higher-than-normal levels of glucose in their blood. Also known as blood sugar.
Goal setting: A behavioral-therapy strategy where you set realistic short-, medium-, and long-term goals to help change eating and activity behaviors.
H
Health care professional (HCP): A medical care provider who works with you to diagnose, treat, or prevent obesity. Sometimes referred to as health care providers. Obesity health care professionals may include endocrinologists, primary care doctors, bariatric surgeons, physician assistants, nurses, nurse practitioners, registered dietitians, physical therapists, psychologists, psychiatrists, and pharmacists.
Healthy eating plan: An eating plan that includes nutrient-rich foods in right-size portions. Generally, a healthy diet is made up of a wide range of nutritious foods, including fruits, vegetables, whole grains, lean meats, poultry, eggs, seafood, low-fat dairy, nuts, seeds, legumes, and healthy fats. It also limits highly processed foods; sugar-sweetened beverages; alcohol; and foods with added sugar, saturated fats, trans fats, or sodium. Examples of healthy diets include the Mediterranean diet, the Dietary Approaches to Stop Hypertension (DASH) eating plan, and the MyPlate Plan.
I
Insulin: A hormone made by your pancreas that controls the level of glucose (sugar) in your blood. If insulin is not made by the pancreas or the body does not respond to it properly, you may develop diabetes.
Internalized weight bias (IWB): Negative attitudes about obesity that people with obesity hold against themselves and others with obesity. IWB can interfere with your opinion of yourself, your quality of life, your relationships, and obesity-related self-care. People with IWB may be less likely to see a health care professional for obesity treatment or follow their treatment plan. It can even hold you back from committing to eating and exercise changes.
L
Laparoscopic adjustable gastric band surgery: A type of obesity surgery that uses an inflatable silicone band around the top part of your stomach to create a smaller stomach pouch with an adjustable opening.
Laparoscopic sleeve gastrectomy: A type of obesity surgery in which much of your stomach is removed.
Liraglutide injection (Saxenda®): A type of weight-management medication that reduces your appetite and helps you feel fuller by slowing down stomach emptying. It's also prescribed to treat diabetes.
Low-calorie diet (LCD): An eating plan that limits the amount of food you eat to about 1,000-1,200 calories per day for women and 1,200-1,600 calories per day for men. An LCD may be made up of food, meal-replacement products, or a mix of both. Talk with your health care professional before starting an LCD.
M
Metabolic syndrome: A group of conditions that raise your risk of serious medical problems such as heart disease, stroke, and diabetes. The risk of metabolic syndrome increases with obesity. Individuals with metabolic syndrome have one or more of the following: high blood pressure (hypertension), high blood sugar, unhealthy cholesterol levels, and extra belly fat. Eating a healthy diet, exercising, and losing weight can help protect you from metabolic syndrome and the medical conditions associated with it. Also known as insulin resistance syndrome.
Muscle-strengthening activity: Exercise or other activity that builds muscle mass and strengthens your muscles. Examples include weightlifting, exercising with resistance bands, and doing exercises such as squats or push-ups that build muscle by using your body weight for resistance. Current activity guidelines for adults recommend two days a week of muscle-strengthening activity that works all major muscle groups (i.e., legs, hips, back, abdomen, chest, shoulders, and arms). Strength training builds muscle mass, which helps increase your metabolic rate (the rate at which you burn calories). It's also very important for your bone health.
N
Naltrexone/bupropion (Contrave®): A type of weight-management medication that reduces your appetite to help you eat less. It's also used to help people stop smoking.
O
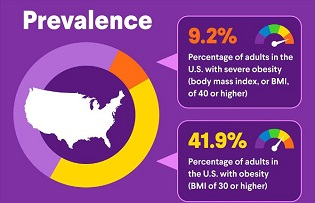
Obesity: A biological, preventable, and treatable disease that means a person has too much body fat. There are different factors that can contribute to a person having obesity, including family history and environment. Health care professionals may use body mass index (BMI) as a way to determine whether you are obese. Someone is considered obese if their BMI is 30 or above. Also known as adiposity-based chronic disease (ABCD).
Obesity-associated cancers: Cancers that have a higher risk of occurring in people who are overweight or have obesity, including cancers of the breast, cervix, colon, esophagus, pancreas, prostate, kidneys, and uterus.
Obesity blood testing: Lab tests that your health care professional may use to look for signs of obesity-related health conditions. Obesity blood testing may include measurement of your cholesterol, liver function, and blood sugar.
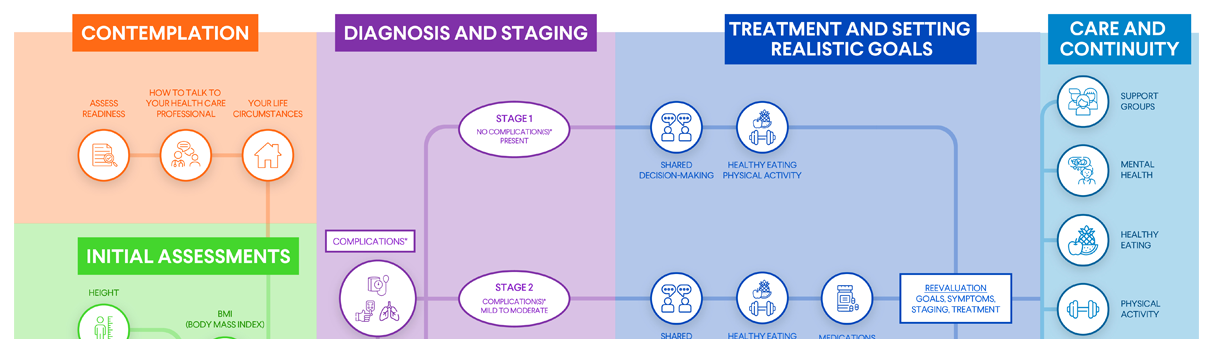
Obesity staging: A process your health care professional uses to determine the impact obesity is having on your health. After doing a physical exam, asking about any symptoms you may have, reviewing your medical history, performing any necessary lab testing, and evaluating any obesity-related health conditions you may have, your health care professional classifies your obesity as stage 1 (obesity with no weight-related complications), stage 2 (obesity with one or more mild to moderate weight-related complications), or stage 3 (obesity with one or more severe weight-related complications). Your obesity stage helps your provider determine what types of treatment to recommend.
Obesity surgery: Any type of surgical procedure performed on the stomach and/or intestines to help bring about long-term weight loss. Also known as bariatric surgery.
Obstructive sleep apnea (OSA): A medical condition where your breathing stops and restarts frequently during the night, starving your body of oxygen and preventing you from getting enough sleep. The risk of OSA is high in individuals with obesity, because airways can become blocked by excess fat in your neck. Losing weight can help reduce OSA symptoms.
Orlistat (Xenical®, Alli®): A type of weight-management medication that blocks the absorption of one-third of the fat in the foods you eat.
Overweight: The condition of weighing more than is healthy for you, but not enough to be considered obesity. Health care professionals may use body mass index (BMI) as a way to determine whether you are overweight. Using BMI, someone is considered overweight if their BMI is between 25 and 30.
P
Patient support groups: Organized groups of patients who live with obesity and support each other through regular meetings and check-ins.
Phentermine/topiramate (Qsymia®): A weight-management medication that decreases your appetite and helps you feel full after eating.
Physical activity: Exercise or other activity that involves moving your body and burning calories, such as walking, jogging, swimming, dancing, water aerobics, playing sports, exercise classes, using a stationary cycle or treadmill, or lifting weights, as well as household chores and other tasks that get you moving. Current guidelines for adults recommend at least 150 minutes of moderate-intensity physical activity each week, including muscle-strengthening activity on two days.
Prediabetes: A medical condition where your blood sugar is higher than normal, but not high enough for a diagnosis of type 2 diabetes. Being overweight or obese significantly raises your risk of developing prediabetes. Many people with prediabetes go on to develop type 2 diabetes. Healthy eating, exercise, and weight loss may prevent or postpone type 2 diabetes in these cases.
R
Registered dietitian: A health care professional who is an expert in food and nutrition and has met certain requirements for education and credentialing. Dietitians can play a key role in managing obesity. They offer individualized support based on your personal lifestyle and goals while also understanding the complexities of the disease. Also known as a registered dietitian nutritionist.
Roux-en-Y gastric bypass: A type of obesity surgery that creates a small stomach pouch that connects directly to your small intestine, bypassing the majority of your stomach and a portion of your upper intestines. Also known as gastric-bypass surgery.
S
Self-monitoring: A behavioral-therapy strategy where you record information about your daily eating and activity and use this information to identify unhelpful habits and make smart choices in the future.
Semaglutide injection (Wegovy®): A type of weight-management medication that reduces your appetite and helps you feel fuller by slowing down stomach emptying. It's also prescribed to treat diabetes.
Social determinants of health (SDOH): Factors outside your body that may affect your health, well-being, and quality of life, such as where you are born, live, learn, and work. SDOH can affect your health, well-being, and quality of life. In many lower socioeconomic communities, SDOH can raise your risk of obesity and other health problems.
Step counter: A device such as a watch or a smartphone app that counts your daily steps and helps you stay committed to exercise. Your health care professional can help you decide on a good daily step goal for you.
Stimulus control: A behavioral-therapy strategy in which you identify things that trigger overeating and use awareness to help manage them.
T
Tirzepatide (Zepbound®): A diabetes drug that was found to bring about weight loss in a clinical trial. It is not yet FDA-approved for obesity, but it is currently undergoing a clinical trial to evaluate safety and efficacy as a weight-management medication in individuals without diabetes.
Type 2 diabetes: A serious disease where you have too much sugar (glucose) in your blood. In type 2 diabetes, the body doesn't respond to insulin properly, and later in the disease the body typically does not make enough insulin. (Insulin is a hormone made by your pancreas that controls the level of glucose in your blood.) Without proper management, type 2 diabetes can lead to serious medical conditions, such as vision loss, nerve damage, and limb loss. Being overweight or obese significantly raises your risk of developing type 2 diabetes. Individuals can manage high blood sugar with healthy eating, exercise, weight loss, and medication (when needed).
V
Very low-calorie diet (VLCD): An eating plan that limits the amount of food you eat to about 800 calories or less per day. Most VLCDs use shakes or other meal-replacement products to make sure you get the nutrients your body needs. Although a VLCD is an option for some individuals, it requires medical supervision and should be followed only if your health care professional recommends it. VLCDs are sometimes recommended before obesity surgery.
W
Waist circumference: A measure that takes into account how much fat you have stored around your waist. A high waist circumference can increase your chance of heart disease and diabetes. Specifically, women with a measure of more than 35 inches and men of more than 40 inches fall into a higher risk category.
Weight-loss assessment: A process your health care professional follows to check your physical and emotional health as they relate to your weight. It includes various check-ins and measurements that seek to quantify the impact of obesity on your health and well-being. These factors include your weight, BMI, waist circumference, weight-related health complications, and stage of obesity.
Weight-management medications: Medications that help you lose weight by reducing your appetite, helping you feel fuller faster after eating, and/or limiting the amount of fat your body absorbs from food.
Weight-related stigmas: Negative and unfair beliefs about people with obesity.
Weight-related bias: Unjust treatment of people with obesity based on negative beliefs.





 DOWNLOAD
DOWNLOAD